A diagnosis of multiple sclerosis can feel overwhelming. Many patients describe the moment they hear the words as life-changing — filled with uncertainty, fear of disability, and countless questions about the future. Will symptoms worsen? Will I lose mobility? Are there treatments that can truly slow or change the course of the disease?
Multiple sclerosis (MS) affects nearly 2.8 million people worldwide, and its unpredictable nature makes it one of the most emotionally challenging neurological disorders. Symptoms can range from mild numbness to severe mobility impairment, vision loss, and cognitive changes. For families, the journey is equally demanding — balancing hope with practical decisions about long-term care.
The good news is that Multiple Sclerosis Treatment Options have advanced significantly over the last two decades. From innovative disease-modifying drugs to cutting-edge stem cell therapy, the landscape of MS treatment is evolving faster than ever before. While there is still no definitive cure, modern therapies aim to reduce relapses, slow progression, protect nerve function, and improve quality of life.
This guide explores conventional treatments, the multiple sclerosis latest treatment breakthroughs, and the growing role of advanced regenerative medicine — helping patients and caregivers make informed decisions with clarity and confidence.
What Is Multiple Sclerosis (MS)?
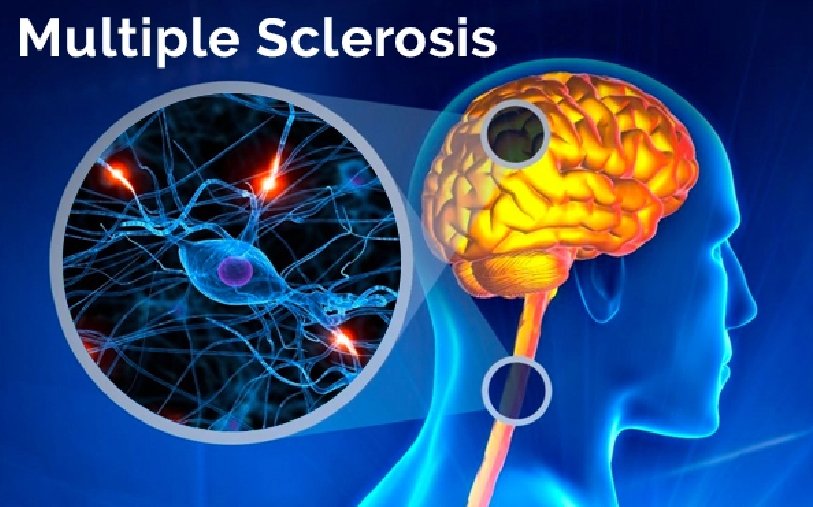
Multiple sclerosis is a chronic autoimmune disorder that affects the central nervous system (brain and spinal cord). In MS, the immune system mistakenly attacks the protective covering of nerve fibers, called myelin. This process — known as demyelination — disrupts communication between the brain and the rest of the body.
Over time, repeated inflammation may lead to permanent nerve damage and scarring (sclerosis).
What Is Multiple Sclerosis (MS)?
Understanding the type of MS is crucial in choosing appropriate Multiple Sclerosis Treatment Options.
1. Clinically Isolated Syndrome (CIS)
A first episode of neurological symptoms lasting at least 24 hours. Not all CIS cases develop into MS, but many do.
2. Relapsing-Remitting MS (RRMS)
The most common form (about 85% of cases at diagnosis). Characterized by clearly defined relapses followed by periods of partial or complete recovery.
3. Secondary Progressive MS (SPMS)
Begins as RRMS but gradually transitions into steady progression with fewer relapses.
4. Primary Progressive MS (PPMS)
Marked by gradual worsening of symptoms from the start, without distinct relapses.
Each type requires a personalized treatment approach.
Discover if Stem Cell Therapy Can Help You!
Book a Free Consultation with Our Experts at Viezec !
Conventional Treatment Options
Modern conventional therapies focus on three primary goals:
-
Reducing relapse frequency
-
Slowing disease progression
-
Managing symptoms
1. Disease-Modifying Therapies (DMTs)
DMTs are the foundation of standard MS management. These medications regulate or suppress immune activity to prevent attacks on myelin.
Common categories include:
-
Injectable medications (interferon beta, glatiramer acetate)
-
Oral medications (fingolimod, dimethyl fumarate, teriflunomide)
-
Infusion therapies (ocrelizumab, natalizumab, alemtuzumab)
These drugs have significantly improved relapse control, particularly for RRMS.
2. Corticosteroids
High-dose steroids are used during acute relapses to reduce inflammation and shorten recovery time. However, they do not alter long-term progression.
3. Immunosuppressants
In aggressive cases, stronger immune-suppressing drugs may be used. These require careful monitoring due to infection risk.
4. Symptom Management
MS symptoms vary widely. Treatment may include:
-
Muscle relaxants for spasticity
-
Physical therapy for mobility
-
Medications for bladder dysfunction
-
Cognitive rehabilitation
-
Fatigue management strategies
Limitations of Conventional Therapies
While current therapies have improved patient outcomes, several challenges remain:
-
Not all patients respond effectively
-
Side effects can be significant
-
Long-term immune suppression increases infection risk
-
Limited impact in progressive MS
-
No reversal of existing nerve damage
This has led researchers to explore advanced MS treatment approaches aimed at immune reset and neuroprotection.
Latest Advances in Multiple Sclerosis Treatment
The field of neurology has seen rapid innovation in recent years.
1. Targeted Immunotherapy
Newer monoclonal antibodies target specific immune cells involved in MS, offering more precise disease control with potentially fewer systemic effects.
2. B-Cell Therapy
Medications targeting B cells (such as ocrelizumab) have shown benefit even in primary progressive MS — a historically difficult subtype to treat.
3. Personalized Medicine
Genetic markers and biomarker research now help tailor therapy to individual disease patterns, improving response rates and minimizing unnecessary exposure to ineffective drugs.
4. Remyelination Research
Scientists are investigating therapies that promote repair of damaged myelin — a potential breakthrough in reversing disability rather than only preventing progression.
5. Stem Cell Therapy for MS
Among the most promising developments is stem cell therapy for MS, particularly hematopoietic stem cell transplantation (HSCT). This approach aims to “reset” the immune system.
Start Your Regenerative Journey Today!
Contact Viezec for Personalized Stem Cell Therapy Plan
Stem Cell Treatment for Multiple Sclerosis
Stem cell therapy represents one of the most discussed and researched advanced MS treatment strategies today. While not considered a universal cure, it has demonstrated encouraging results in carefully selected patients.
How Does Stem Cell Therapy Work in MS?
MS is driven by an abnormal immune response. Stem cell therapy aims to:
-
Eliminate malfunctioning immune cells
-
Rebuild a healthier immune system
-
Reduce further autoimmune attacks
In some approaches, stem cells may also promote tissue repair and reduce inflammation.
Types of Stem Cells Used
1. Hematopoietic Stem Cells (HSCT)
The most established method. These stem cells are derived from the patient’s own bone marrow or blood.
Goal:
Reset the immune system after high-dose chemotherapy removes abnormal immune cells.
2. Mesenchymal Stem Cells (MSCs)
Derived from bone marrow, adipose tissue, or umbilical sources.
Potential benefits:
-
Anti-inflammatory properties
-
Immune modulation
-
Support for tissue repair
Research is ongoing to confirm long-term outcomes.
Step-by-Step Stem Cell Treatment Procedure (HSCT Model)
While protocols vary by hospital, a typical process includes:
Step 1: Evaluation and Eligibility Assessment
Comprehensive neurological exams, MRI scans, blood tests, and cardiac screening.
Step 2: Stem Cell Collection
Patient’s stem cells are harvested from blood after stimulation.
Step 3: Conditioning Therapy
Chemotherapy is administered to suppress or eliminate the abnormal immune system.
Step 4: Stem Cell Infusion
Previously collected stem cells are infused intravenously.
Step 5: Recovery and Monitoring
Immune system gradually rebuilds over weeks to months.
The entire process may require hospitalization for several weeks.
Safety Profile and Expected Outcomes
Stem cell therapy is intensive and must be performed in specialized centers. Potential benefits include:
-
Reduced relapse rates
-
Stabilization of disease
-
Possible improvement in disability in early-stage aggressive MS
However, risks include:
-
Infection
-
Temporary infertility
-
Chemotherapy-related complications
-
Rare but serious immune reactions
Long-term follow-up studies show promising remission rates in selected patients, particularly those with active relapsing MS who failed conventional DMTs.
Stem Cell Therapy vs Conventional Treatment
| Aspect | Conventional DMTs | Stem Cell Therapy |
|---|---|---|
| Goal | Control immune response | Reset immune system |
| Frequency | Ongoing medication | One-time intensive procedure |
| Best for | Early RRMS | Aggressive RRMS |
| Risks | Chronic immune suppression | Short-term intensive risks |
| Cure? | No | No guaranteed cure |
Stem cell therapy is not first-line treatment but may be considered in specific, carefully selected cases.
Who Is an Ideal Candidate?
Clinical Criteria
-
Diagnosed with aggressive RRMS
-
Frequent relapses despite DMTs
-
Evidence of active inflammation on MRI
-
Relatively early in disease course
-
Adequate organ function
Non-Clinical Considerations
-
Psychological readiness
-
Strong support system
-
Ability to comply with follow-up
Progressive MS without inflammatory activity may not benefit as much.
Is Your Condition Eligible for Stem Cell Therapy?
Speak directly with our specialist.
Why Choose Advanced Stem Cell Treatment Abroad?
Many international patients explore treatment overseas due to:
1. Cost Advantage
Stem cell procedures can be significantly more affordable in certain countries without compromising quality.
2. Advanced Protocols
Some international centers specialize in HSCT with experienced multidisciplinary teams.
3. Comprehensive Care
Dedicated transplant units and post-procedure rehabilitation programs.
Medical tourism facilitators such as Viezec Medical Tourism support patients in identifying accredited hospitals, arranging consultations, coordinating travel, and ensuring ethical medical guidance. Rather than promoting treatment blindly, responsible facilitators prioritize transparent information, hospital partnerships, and patient-centered decision-making.
Choosing treatment abroad requires thorough research, second opinions, and confirmation of regulatory standards.
Frequently Asked Questions
1. What are the most effective Multiple Sclerosis Treatment Options today?
Disease-modifying therapies remain first-line treatment. In aggressive cases, stem cell therapy may be considered after specialist evaluation.
2. Is stem cell therapy a cure for MS?
No. There is currently no guaranteed cure for MS. Stem cell therapy may induce long-term remission in selected patients but does not eliminate the disease entirely.
3. Who qualifies for stem cell therapy for MS?
Typically patients with active relapsing MS who have not responded to standard treatments and meet strict medical eligibility criteria.
4. What is the multiple sclerosis latest treatment breakthrough?
Advances include B-cell targeted therapies, personalized medicine approaches, and continued research into remyelination and regenerative treatments.
5. Is stem cell treatment safe?
When performed in accredited hospitals by experienced teams, it can be safe for appropriate candidates. However, it carries significant short-term risks and requires careful monitoring.
6. How long does recovery take after HSCT?
Initial hospitalization may last several weeks, while immune recovery can take months. Regular follow-up is essential.
7. Can progressive MS be reversed?
Currently, most therapies aim to slow progression rather than reverse established nerve damage. Research into repair strategies continues.
A Hopeful Yet Realistic Future
Living with multiple sclerosis requires resilience, informed decision-making, and access to expert care. The landscape of Multiple Sclerosis Treatment Options has evolved dramatically — offering patients more control and more hope than ever before.
From advanced disease-modifying therapies to innovative stem cell protocols, treatment today is no longer limited to symptom management alone. However, each option must be evaluated carefully, balancing potential benefits with risks.
If you or a loved one is exploring advanced MS treatment, the most important step is consultation with an experienced neurologist. A personalized approach — grounded in science, transparency, and ethical care — offers the best path forward.
MS may be unpredictable, but progress in medical science is steady. With informed choices and the right medical guidance, many patients continue to lead active, meaningful lives — redefining what is possible after diagnosis.