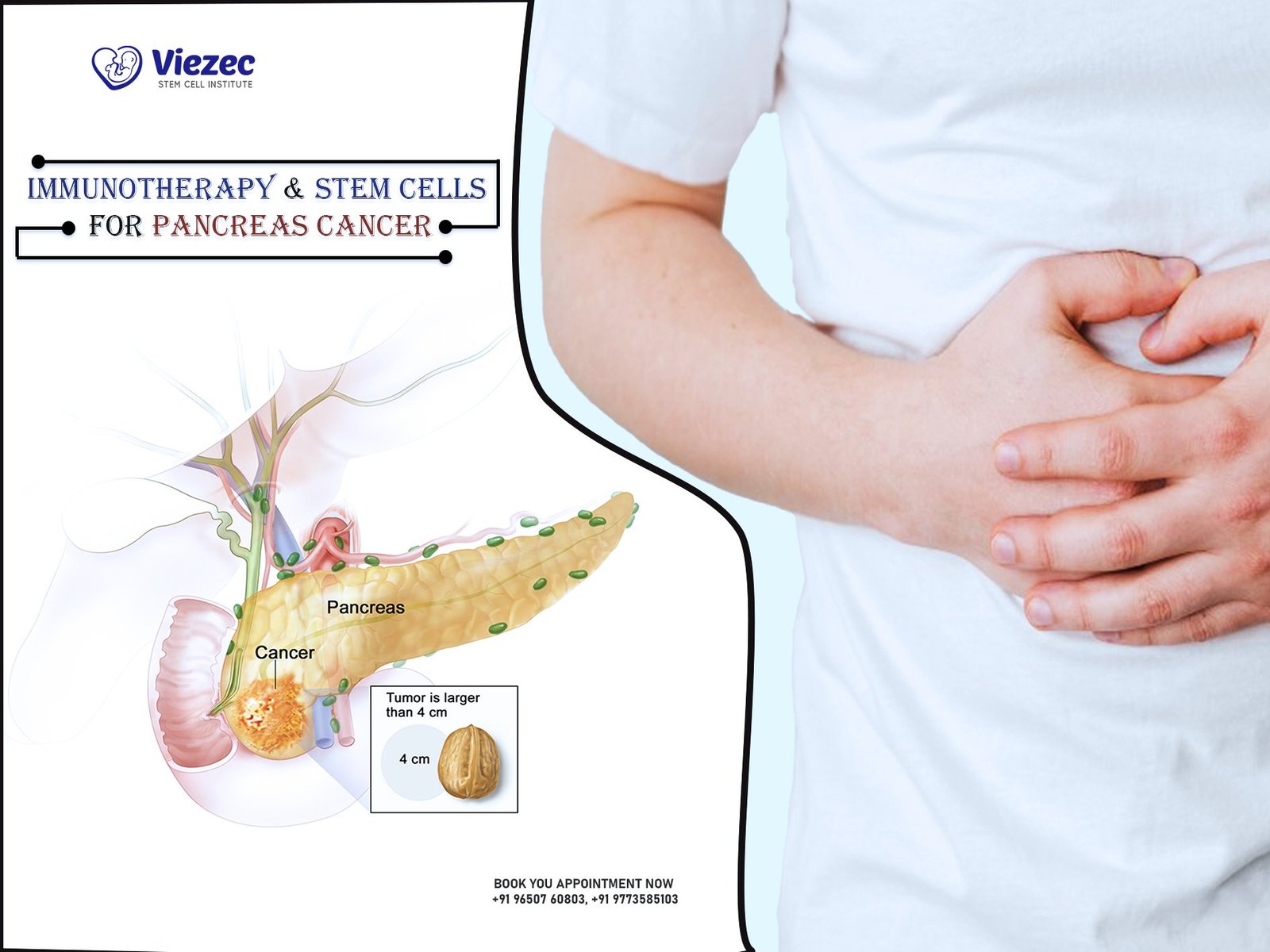
Pancreatic cancer, often referred to as the “silent killer,” is notorious for its aggressive nature and limited treatment options. The pancreas, a vital organ nestled deep within our abdomen, plays a crucial role in digestion and blood sugar regulation. When cancer strikes this organ, it tends to remain hidden until it reaches an advanced stage, making early detection a daunting challenge.
Traditionally, treatments like surgery, chemotherapy, and radiation therapy have been the go-to options. However, they often come with debilitating side effects and varying success rates. This grim reality has driven researchers and medical professionals to explore innovative approaches, and two stand out prominently: immunotherapy and stem cell therapy.
Immunotherapy, a groundbreaking method in the world of cancer treatment, capitalizes on our own immune system’s power to fight cancer cells. Unlike traditional treatments that directly target the tumor, immunotherapy enhances the body’s natural defenses, offering a ray of hope for pancreatic cancer patients.
On the other front, stem cell therapy enters the scene, leveraging the regenerative potential of stem cells to tackle cancer’s unrelenting growth. When these two cutting-edge therapies join forces, remarkable possibilities emerge, promising more effective treatments with fewer side effects.
In this comprehensive blog, we will delve deep into the world of “Immunotherapy & Stem Cells for Pancreas Cancer.” We will explore the science behind these treatments, their current status in pancreas cancer management, patient success stories, and the exciting future they hold. If you or a loved one is battling this formidable foe, read on, as we embark on a journey of hope, innovation, and a brighter future in the fight against pancreatic cancer.
Introduction to Pancreas Cancer
Overview of Pancreatic Cancer
Pancreatic cancer begins in the pancreas, a vital organ located behind the stomach. It is known for its aggressive nature and low survival rates. The pancreas plays a crucial role in digestion and blood sugar regulation, making early detection and effective treatment essential.
Challenges in Treating Pancreatic Cancer
Pancreatic cancer is often diagnosed at an advanced stage, making it challenging to treat. The tumor’s location in the pancreas and its rapid spread to surrounding tissues pose significant obstacles to successful treatment.
Traditional Treatment Approaches
Traditional treatment options for pancreatic cancer include:
Surgery
Surgery aims to remove the tumor or part of the pancreas. It is most effective when the cancer is localized and has not spread to other organs.
Chemotherapy
Chemotherapy uses drugs to target and kill cancer cells. It is often used in combination with surgery or radiation therapy.
Radiation Therapy
Radiation therapy uses high-energy rays to target and destroy cancer cells. It is sometimes used before surgery to shrink tumors.
Promise of Immunotherapy
What is Immunotherapy?
Immunotherapy is a revolutionary approach to cancer treatment that harnesses the body’s immune system to fight cancer cells. It differs from traditional treatments by boosting the body’s natural defenses.
How Does Immunotherapy Work?
Immunotherapy works by stimulating the immune system to recognize and attack cancer cells. It can be tailored to target specific cancer markers, minimizing damage to healthy cells.
Benefits of Immunotherapy for Cancer Treatment
Immunotherapy offers several advantages, including fewer side effects compared to chemotherapy and radiation. It also has the potential for long-term remission.
Immunotherapy and Pancreas Cancer
Current Status of Immunotherapy in Pancreas Cancer
Immunotherapy has shown promise in treating various cancers, but its effectiveness in pancreatic cancer is still being explored through ongoing clinical trials.
Clinical Trials and Research Findings
Researchers are continually investigating new immunotherapies and combinations to improve outcomes for pancreatic cancer patients.
Stem Cells in Cancer Treatment
Understanding Stem Cells
Stem cells are undifferentiated cells with the potential to develop into various cell types. They play a crucial role in tissue regeneration and repair.
Role of Stem Cells in Cancer Growth
Some cancer cells exhibit characteristics similar to stem cells, contributing to tumor growth and resistance to treatment.
Stem Cells and Pancreatic Cancer
The Potential of Stem Cells in Treating Pancreatic Cancer
Researchers are studying the use of stem cells to target and eliminate cancer cells in pancreatic tumors, potentially offering a new avenue for treatment.
Ongoing Research and Developments
Ongoing research aims to better understand the role of stem cells in pancreatic cancer and how they can be harnessed for therapy.
Combining Immunotherapy and Stem Cells
Synergy Between Immunotherapy and Stem Cell Therapy
Combining the regenerative properties of stem cells with the precision of immunotherapy holds great promise in enhancing treatment outcomes for pancreatic cancer patients.
Advantages and Challenges
While the combination of these therapies offers exciting possibilities, challenges such as optimal dosing and potential side effects must be addressed.
Patient Success Stories
Real-life stories of individuals who have experienced positive outcomes through immunotherapy and stem cell treatments provide hope and inspiration to others.
Future of Pancreatic Cancer Treatment
Advancements in personalized medicine, early detection methods, and innovative therapies are paving the way for a more optimistic outlook in the fight against pancreatic cancer.
Costs and Accessibility
Understanding the costs associated with these treatments and the accessibility of cutting-edge therapies is crucial for patients and their families.
Considerations for Patients
Determining who is eligible for immunotherapy and stem cell therapy, as well as potential side effects and risks, is essential for informed decision-making.
The Role of Clinical Trials
Clinical trials play a vital role in advancing the field of pancreatic cancer treatment. Patients should consider participating to contribute to ongoing research.
Expert Opinions
Leading oncologists and researchers in the field provide insights into the current state of immunotherapy and stem cell therapy for pancreatic cancer.
The landscape of pancreatic cancer treatment is evolving rapidly, offering new hope and possibilities for patients. Combining the power of immunotherapy and stem cell therapy represents a promising frontier in the fight against this challenging disease.
Frequently Asked Questions
- What is the success rate of immunotherapy for pancreatic cancer?
- The success rate of immunotherapy for pancreatic cancer varies, but it has shown promise in improving outcomes, particularly in some patients with advanced stages. Success rates can depend on individual factors, including the stage of cancer and the patient’s overall health.
- Are there any potential side effects of stem cell therapy in pancreatic cancer treatment?
- Stem cell therapy may have side effects, which can vary from person to person. Common side effects may include fatigue, fever, and mild discomfort at the injection site. It’s essential to discuss potential risks with your healthcare team.
- How can I find clinical trials for pancreatic cancer treatment near me?
- You can find clinical trials for pancreatic cancer treatment near you by consulting with your oncologist or using reputable online resources such as the National Cancer Institute’s clinical trials database. Your healthcare team can guide you through the process of enrolling in a suitable trial.
- Is immunotherapy covered by health insurance plans?
- Immunotherapy is often covered by health insurance plans, but coverage can vary depending on your specific plan and the type of immunotherapy prescribed. It’s crucial to check with your insurance provider and healthcare team to understand your coverage and potential costs.
- What are the long-term prospects for patients who undergo these innovative therapies?
- The long-term prospects for patients undergoing immunotherapy and stem cell therapy for pancreatic cancer are continually evolving as research progresses. Some patients have achieved long-term remission and improved quality of life. However, individual outcomes can vary, and it’s essential to discuss expectations with your healthcare provider based on your unique circumstances.