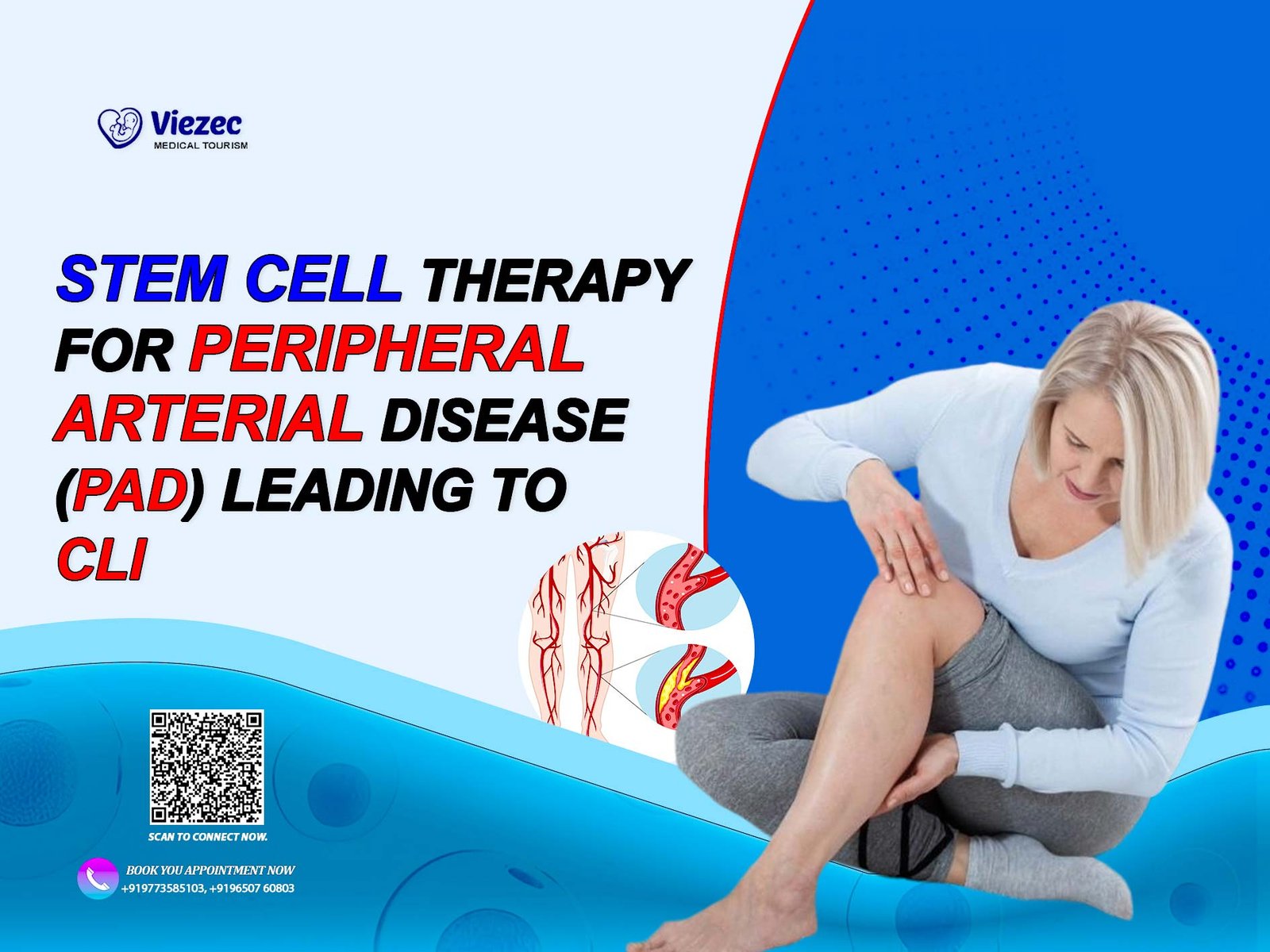
Peripheral Arterial Disease (PAD) is a progressive vascular condition that reduces blood flow to the limbs due to narrowing or blockage of arteries. In advanced stages, it can progress to Critical Limb Ischemia (CLI), a severe form of PAD characterized by chronic pain, non-healing wounds, and a high risk of limb loss. Around the world, PAD is increasingly recognized as a major cause of disability, especially among patients with diabetes, smoking history, and cardiovascular disease.
In recent years, regenerative medicine has introduced a new direction in treatment strategies. Among these, stem cell therapy has emerged as a promising supportive approach for patients with advanced PAD and CLI who have limited response to conventional treatments. This therapy focuses on improving blood circulation and tissue repair through the body’s own regenerative mechanisms rather than purely mechanical or surgical intervention.
Understanding Peripheral Arterial Disease (PAD)
Peripheral Arterial Disease develops when fatty deposits, known as atherosclerotic plaques, accumulate inside the arteries and restrict blood flow. This reduced circulation most commonly affects the legs, although it can also impact other parts of the body. Over time, tissues deprived of oxygen and nutrients begin to deteriorate, leading to pain and functional impairment.
The causes of PAD are usually linked to systemic vascular risk factors. Smoking is one of the strongest contributors, as it damages blood vessel walls and accelerates plaque formation. Diabetes also plays a major role by affecting microvascular circulation and nerve function. High blood pressure, high cholesterol, obesity, and sedentary lifestyle further increase the risk.
Symptoms of PAD often begin subtly. Many patients experience leg fatigue, cramping while walking, or a sensation of heaviness that improves with rest. This stage is commonly known as intermittent claudication. As the disease progresses, pain may occur even at rest, signaling a more advanced stage of ischemia. Without timely intervention, PAD can progress into Critical Limb Ischemia.
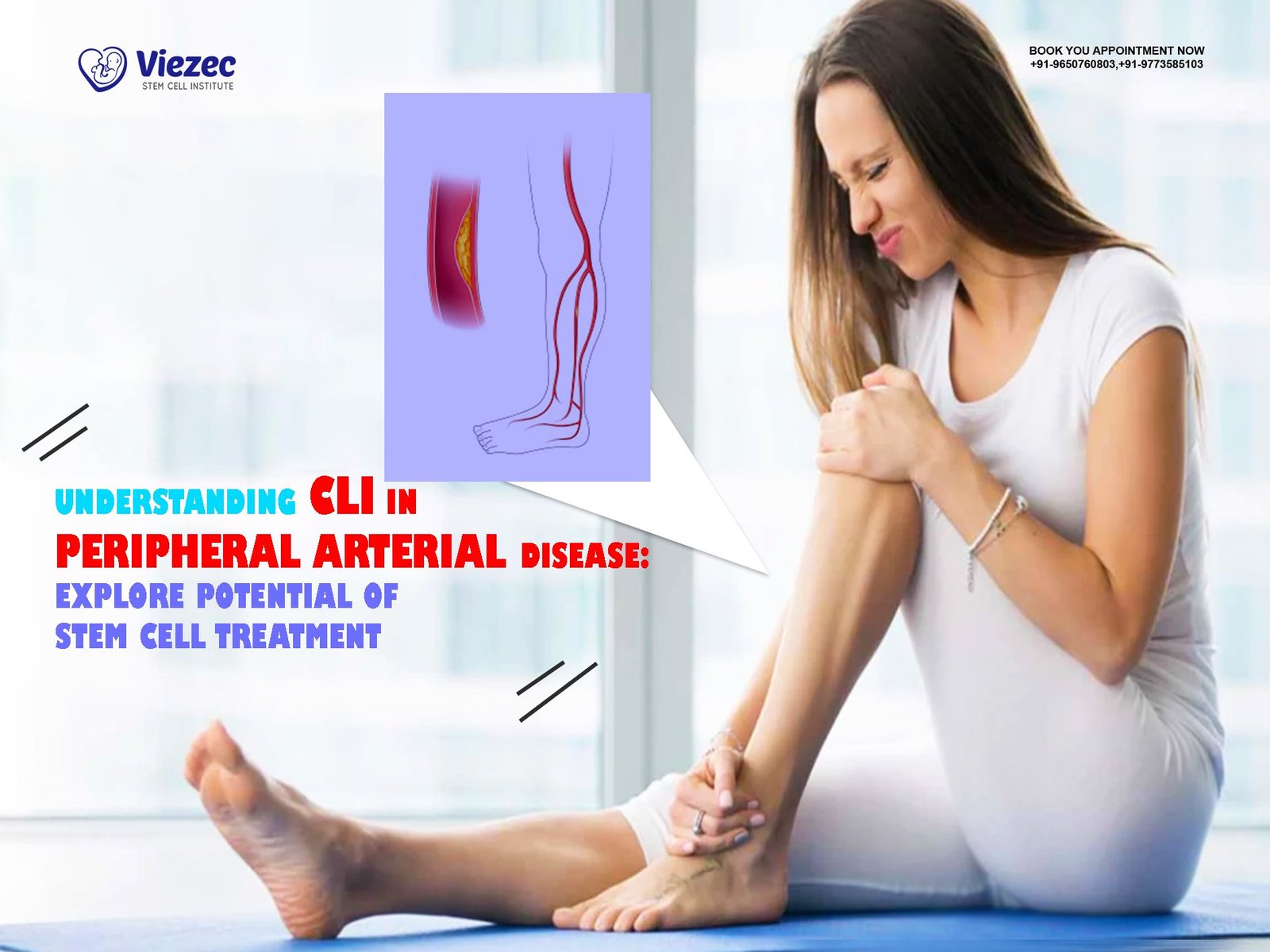
What is Critical Limb Ischemia (CLI)?
Critical Limb Ischemia represents the most severe form of PAD. At this stage, blood flow is significantly reduced, and tissues in the lower limbs are no longer receiving adequate oxygen even at rest. This condition is not only painful but also limb-threatening.
Patients with CLI often experience persistent pain in the feet or legs, especially at night. Small injuries or cuts fail to heal properly and may develop into chronic ulcers. In some cases, the skin may turn dark or develop gangrene due to tissue death. The risk of amputation increases significantly if blood flow is not restored.
CLI is considered a medical emergency because it reflects advanced systemic vascular disease. Beyond limb loss, it also indicates a higher risk of cardiovascular events such as heart attack and stroke. Therefore, early recognition and intervention are critical.
Limitations of Conventional Treatments
Standard treatment approaches for PAD and CLI focus primarily on improving blood flow and managing symptoms. Medications such as antiplatelet agents, statins, and vasodilators are commonly prescribed to reduce clot formation and improve circulation. While these can slow disease progression, they often do not reverse advanced vascular damage.
In more severe cases, interventional procedures such as angioplasty or stenting are performed to physically open narrowed arteries. Surgical bypass may also be considered to reroute blood flow around blocked vessels. Although these procedures can be effective, they are not suitable for all patients.
Many individuals with CLI are poor candidates for surgery due to diffuse vascular disease, diabetes-related complications, or overall health limitations. Even after successful procedures, restenosis or re-blockage of arteries can occur over time. This creates a need for additional therapeutic strategies that go beyond mechanical restoration of blood flow.
What is Stem Cell Therapy for PAD?
Stem cell therapy is a regenerative medical approach that uses the body’s own repair system to promote healing. Stem cells are unique because they have the ability to develop into different types of cells and support tissue regeneration. In the context of PAD, the goal is to stimulate the formation of new blood vessels and improve circulation in ischemic tissues.
Rather than directly opening blocked arteries, stem cell therapy works at a biological level. It encourages angiogenesis, which is the formation of new microvessels that can bypass blocked regions and restore oxygen supply to affected tissues. This can potentially improve limb function and reduce ischemic pain in patients with advanced disease.
The therapy typically involves harvesting stem cells from the patient’s own bone marrow or peripheral blood. These cells are then processed and reintroduced into areas affected by poor circulation, where they begin releasing growth factors and signaling molecules that support healing.
Discover if Stem Cell Therapy Can Help You!
Book a Free Consultation with Our Experts at Viezec !
How Stem Cell Therapy Works in PAD and CLI
The mechanism of stem cell therapy in PAD and CLI is primarily centered on regeneration and vascular repair. Once introduced into the affected region, stem cells release a variety of bioactive compounds that stimulate tissue healing. These include growth factors that encourage the development of new blood vessels and improve oxygen delivery.
One of the key processes involved is neovascularization. This refers to the growth of new capillaries that help bypass blocked arteries. Over time, this improved microcirculation can reduce pain and enhance tissue survival in ischemic areas.
Stem cells also help reduce inflammation, which is a major contributor to vascular damage. By modulating the inflammatory response, they create a more favorable environment for healing. In some cases, patients may experience gradual improvement in walking distance, reduction in rest pain, and better wound healing.
The procedure is generally performed using minimally invasive techniques. Depending on the protocol, stem cells may be administered through intramuscular injections in the affected limb or intravenously to allow systemic distribution. The approach is carefully tailored based on the severity of the condition.
Benefits of Stem Cell Therapy for PAD
Stem cell therapy provides a regenerative approach that may support improved circulation and limb function in patients with advanced Peripheral Arterial Disease (PAD) and Critical Limb Ischemia (CLI).
- Minimally invasive procedure with no major surgical cuts or arterial reconstruction
- Promotes new blood vessel formation to improve blood circulation naturally
- Helps reduce ischemic pain associated with poor limb oxygen supply
- Supports better wound healing in chronic non-healing ulcers
- May reduce risk of amputation in selected advanced cases
- Improves mobility and overall quality of life in many patients
Who Can Benefit from Stem Cell Therapy?
Stem cell therapy is generally considered for patients with advanced PAD who have limited response to conventional treatment options. It is particularly relevant for individuals diagnosed with Critical Limb Ischemia who are not suitable candidates for surgical bypass or angioplasty.
Patients with diabetes-related vascular complications often fall into this category, as microvascular damage can make traditional interventions less effective. Similarly, individuals with diffuse arterial blockages or multiple comorbidities may also benefit from regenerative approaches.
However, suitability must always be determined through careful medical evaluation. Not all patients are ideal candidates, and outcomes may vary depending on the severity of disease and overall health condition.
Risks and Safety Considerations
Stem cell therapy is generally considered safe when performed under proper clinical protocols. Since many treatments use autologous stem cells, meaning they are derived from the patient’s own body, the risk of immune rejection is minimal.
Some patients may experience mild and temporary side effects such as localized discomfort at the injection site, mild fever, or fatigue. These effects usually resolve without intervention.
Despite its safety profile, stem cell therapy is still an evolving field. It is important that treatment is conducted in a controlled medical environment with appropriate ethical and clinical standards. Patients should also have realistic expectations, as outcomes can vary.
Start Your Regenerative Journey Today!
Contact Viezec for Personalized Stem Cell Therapy Plan
Current Research and Clinical Evidence
Research into stem cell therapy for Peripheral Arterial Disease (PAD) and Critical Limb Ischemia (CLI) has expanded significantly over the past decade. Clinical studies have explored its potential to improve limb perfusion, enhance microcirculation, reduce ischemic pain, and support ulcer healing in patients with advanced vascular disease. Several clinical trials and systematic reviews have reported encouraging improvements in blood flow and limb function in selected patient groups, particularly those with severe or no-option CLI.
While the results are promising, stem cell therapy is still considered an emerging and investigational treatment rather than a fully established standard of care. Evidence from multiple studies shows mixed outcomes, where some patients experience significant improvement in walking distance, pain reduction, and wound healing, while others show only modest or limited benefits depending on disease severity, comorbidities, and progression of ischemia. (https://pmc.ncbi.nlm.nih.gov/articles/PMC6528204/)
Ongoing clinical trials continue to evaluate the most effective stem cell types, optimal dosage, and delivery methods for vascular regeneration. Researchers are also studying combination approaches that integrate stem cell therapy with growth factors and gene-based therapies to further enhance angiogenesis and tissue repair mechanisms. These evolving strategies aim to improve consistency of outcomes and long-term limb salvage rates in patients with critical limb ischemia. (https://pmc.ncbi.nlm.nih.gov/articles/PMC5994285/)
Recovery and Expected Outcomes
Recovery after stem cell therapy is generally quick, as the procedure is minimally invasive. Most patients can resume normal activities within a short period. However, biological improvement occurs gradually as the body responds to regenerative signals.
Noticeable changes such as reduced pain or improved wound healing may take several weeks to months. In some cases, improvements continue over an extended period as new microvascular networks develop.
It is important to understand that stem cell therapy is not an instant cure. Instead, it should be viewed as a supportive regenerative treatment aimed at improving circulation and slowing disease progression.
Stem Cell Therapy vs Conventional Treatments
Peripheral Arterial Disease (PAD) is traditionally managed through medications and vascular procedures that aim to improve blood flow or reduce symptoms. In contrast, stem cell therapy focuses on repairing damaged tissues and stimulating new blood vessel growth at a biological level, offering a regenerative approach for advanced cases where conventional options may be limited.
Both approaches play an important role in PAD management, but they differ significantly in mechanism, purpose, and long-term impact on vascular health.
| Aspect | Conventional Treatments | Stem Cell Therapy |
|---|---|---|
| Primary Goal | Restore or bypass blood flow mechanically | Regenerate blood vessels and improve microcirculation |
| Approach | Medications, angioplasty, stenting, bypass surgery | Cellular regeneration and tissue repair |
| Mechanism | Opens or reroutes blocked arteries | Stimulates angiogenesis (new blood vessel formation) |
| Focus Area | Large vessel blockages | Microvascular and tissue-level healing |
| Suitability | Early to advanced PAD depending on condition | Mostly advanced PAD / CLI or non-surgical candidates |
| Invasiveness | Can be minimally invasive or surgical | Minimally invasive biological procedure |
| Outcome | Symptom relief and improved blood flow | Potential long-term regenerative improvement |
| Limitations | May not address microvascular damage or recurrence | Still emerging therapy with variable outcomes |
Is Your Condition Eligible for Stem Cell Therapy?
Speak directly with our specialist.
Stem Cell Therapy for PAD in India: A Medical Tourism Perspective
India has emerged as a significant destination for advanced regenerative medicine, particularly for patients seeking stem cell therapy for complex conditions such as Peripheral Arterial Disease (PAD) and Critical Limb Ischemia (CLI). The country offers a combination of modern medical infrastructure, experienced specialists in regenerative medicine, and comparatively lower treatment costs, making it accessible for international patients.
Many patients from regions such as the Middle East, Africa, Southeast Asia, and Europe explore India when conventional treatments in their home countries are either unavailable, unaffordable, or have limited success. In this context, India provides an alternative pathway where patients can access emerging therapies under clinical supervision in specialized medical centers.
Regenerative medicine programs in India typically follow international safety protocols. Stem cell therapy procedures are performed in controlled environments with strict screening, processing, and administration standards. This ensures that patients receive care aligned with global medical guidelines while benefiting from advanced biological treatment approaches.
Frequently Asked Questions
Stem cell therapy has shown encouraging results in improving circulation and reducing symptoms in some patients, especially those with advanced disease. However, effectiveness can vary depending on individual conditions.
Stem cell therapy may help improve blood flow and reduce the severity of symptoms, but complete reversal of CLI is not guaranteed. It is considered a supportive treatment rather than a cure.
Improvements typically develop gradually over several weeks to months as new blood vessels form and tissue repair progresses.
The procedure is minimally invasive and usually well tolerated. Mild discomfort may occur at injection sites but is temporary.
Patients with certain severe infections, advanced organ failure, or specific medical contraindications may not be suitable candidates.
Conclusion
Peripheral Arterial Disease and Critical Limb Ischemia represent serious vascular conditions that can significantly impact quality of life and limb health. While conventional treatments remain the foundation of care, they may not always be sufficient in advanced cases.
Stem cell therapy offers a promising regenerative approach aimed at improving blood flow, supporting tissue repair, and enhancing limb viability. Although still an evolving field, growing clinical evidence suggests its potential as a valuable adjunct in the management of advanced PAD.
For patients exploring innovative treatment options, regenerative medicine provides hope where traditional approaches may have limitations. Organizations such as viezec.com focus on advancing these therapies for patients worldwide through carefully structured clinical protocols and personalized care approaches.
As research continues to evolve, stem cell therapy may play an increasingly important role in the future of vascular disease management, offering new possibilities for patients facing the challenges of PAD and CLI.
Disclaimer
This article is for informational and educational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional before making any decisions regarding diagnosis or treatment.
List of References
Autologous Stem Cell Therapy in PAD – Systematic Review & Meta-analysis of RCTs
https://pubmed.ncbi.nlm.nih.gov/31113463/
Stem Cell Therapy in Critical Limb Ischemia – Meta-analysis of RCTs
https://pubmed.ncbi.nlm.nih.gov/29977308/
Autologous Stem Cell Therapy for PAD – Systematic Review (Stem Cell Research & Therapy)
https://stemcellres.biomedcentral.com/articles/10.1186/s13287-019-1254-5
Clinical Trial Evidence Overview – Adult Stem Cell Therapy in PAD
https://pmc.ncbi.nlm.nih.gov/articles/PMC3846073/
Phase III Clinical Trial Example (Mesenchymal Stem Cells in CLI due to PAD)