Imagine a condition that strikes without warning, creeping stealthily into your life, and threatening not just your mobility but your very limb itself. This is the reality of Critical Limb Ischemia (CLI), a vascular disorder that often remains unnoticed until it reaches a critical stage. In this blog, we shine a spotlight on this silent but deadly assailant of our limbs.
CLI is a condition where blood flow to the extremities, particularly the legs, is severely compromised. It doesn’t announce its presence with blaring sirens; instead, it stealthily chips away at your limb’s vitality. What makes CLI even more insidious is its association with underlying health issues like diabetes, high blood pressure, and smoking, making it a potential threat to many.
Join us on this journey to unveil the mysteries of CLI. From understanding its causes and symptoms to exploring treatment options and emphasizing the pivotal role of timely intervention, we’ll equip you with knowledge to safeguard your limbs and quality of life. Don’t let the “silent killer” claim your vitality – let’s uncover its secrets together.
Understanding Critical Limb Ischemia
Critical Limb Ischemia (CLI) is a complex and potentially life-altering condition that demands our attention and comprehension. At its core, CLI signifies a dire shortage of blood flow to the extremities, particularly the legs, creating a perilous scenario of oxygen and nutrient deprivation. This condition is often the severe endgame of peripheral artery disease (PAD), wherein the arteries responsible for supplying blood to the limbs become severely obstructed.
CLI doesn’t discriminate; it can affect anyone, but certain risk factors such as smoking, diabetes, hypertension, and high cholesterol levels elevate the stakes. To understand CLI is to recognize its multifaceted nature, from its insidious onset to the debilitating consequences it can unleash if neglected.
Recognizing the Warning Signs
Critical Limb Ischemia (CLI) may be a silent invader, but it does leave subtle clues that, if heeded, can make all the difference. Understanding these warning signs is akin to deciphering a hidden language that our limbs speak when they’re in distress.
Pain and Discomfort: CLI often manifests as severe leg pain, particularly during rest. This pain is relentless and unforgiving, serving as a cry for help from oxygen-deprived tissues.
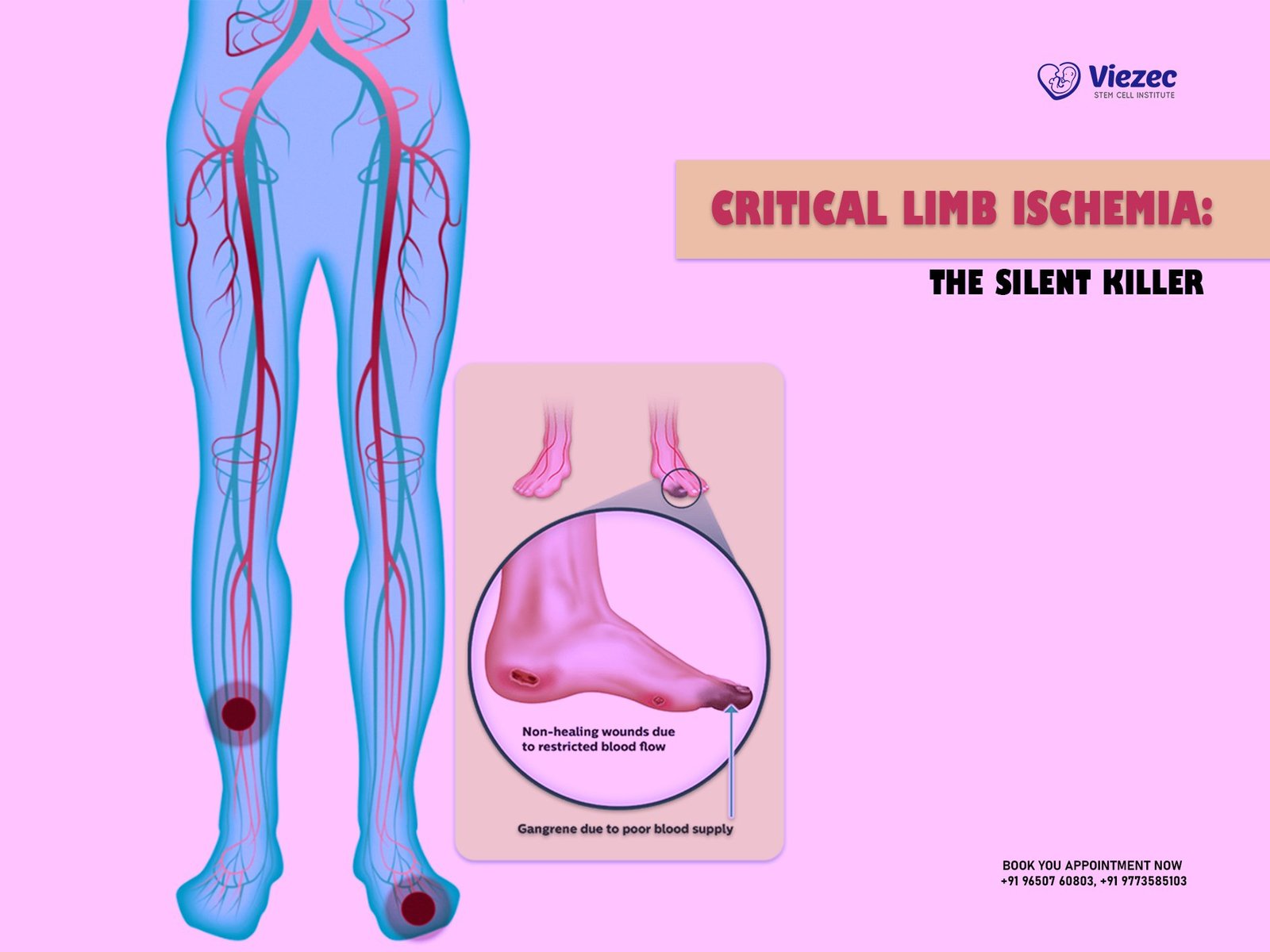
Skin Changes: The skin on affected limbs may exhibit pallor, become cool to the touch, or develop a bluish tint. In more advanced cases, ulcers or sores that refuse to heal can emerge, signaling a dire need for attention.
Impaired Wound Healing: Pay close attention to wounds on your feet or toes. If they take an unusually long time to heal or seem to worsen, this could be a sign of compromised blood flow.
CLI thrives in the shadows, often evading immediate detection. However, by recognizing these subtle hints, you can unmask its presence and take swift action.
Consequences of Neglect
Ignoring the warning signs of Critical Limb Ischemia (CLI) can lead to dire consequences, turning a seemingly benign condition into a life-threatening ordeal. CLI, if left unattended, can be nothing short of a ticking time bomb for your limbs and overall health.
Gangrene and Tissue Loss: CLI’s relentless assault on blood flow can lead to gangrene, a condition where body tissues die due to insufficient oxygen and nutrients. Gangrene is a dire situation that often necessitates amputation to prevent the spread of infection.
Infection and Sepsis: Compromised limbs are vulnerable to infections that can escalate rapidly. When these infections infiltrate the bloodstream, they trigger sepsis, a systemic and potentially fatal response to infection.
Understanding the gravity of CLI’s consequences is crucial. It’s not merely about losing a limb; it’s about preserving your vitality and overall well-being. In the subsequent sections, we’ll explore how to diagnose and treat CLI, emphasizing the importance of timely intervention in preventing these catastrophic outcomes.
Diagnosis and Evaluation
Diagnosing Critical Limb Ischemia (CLI) is a multifaceted process that combines medical history, physical examination, and specialized tests.
Medical History and Physical Examination: A healthcare provider will meticulously review your medical history, including risk factors and symptoms. A comprehensive physical examination assesses the limb’s pulse, skin condition, and any signs of ulcers or wounds.
Non-Invasive Tests: Non-invasive tests like the ankle-brachial index (ABI) and duplex ultrasound help evaluate blood flow and pinpoint blockages in the arteries.
Angiography: In some cases, angiography may be necessary to obtain detailed images of blood vessels, aiding in precise diagnosis and treatment planning.
These diagnostic steps are vital in determining the severity of CLI and guiding appropriate intervention.
Treatment Options
Managing Critical Limb Ischemia (CLI) requires a tailored approach, often involving a combination of strategies to restore blood flow and prevent further complications.
Lifestyle Changes: Lifestyle modifications are paramount. Smoking cessation, a heart-healthy diet, regular exercise, and weight management can reduce risk factors and improve overall vascular health.
Medications: Medications may be prescribed to manage underlying conditions like high blood pressure, diabetes, and high cholesterol, contributing to improved blood flow.
Angioplasty and Stenting: Minimally invasive procedures like angioplasty, where narrowed arteries are widened, and stenting, which involves placing a metal mesh to keep arteries open, can help restore blood flow.
Bypass Surgery: In severe cases, bypass surgery may be necessary to create alternative routes for blood to reach the affected limb.
Treatment choices depend on the individual’s condition and should be discussed with a healthcare provider to determine the most suitable approach. Early intervention is crucial to prevent amputation and improve quality of life.
Importance of Timely Intervention
Timely intervention in cases of Critical Limb Ischemia (CLI) can be the difference between preserving a limb and facing amputation. CLI is a progressive condition, and delaying treatment can lead to irreversible consequences.
Preventing Amputations: Swift action can prevent the need for limb amputation, which is often the last resort when tissue damage becomes severe. Early intervention can halt the progression of CLI, potentially saving the limb.
Improving Quality of Life: Timely treatment can significantly improve the patient’s quality of life. Relief from debilitating pain, enhanced mobility, and the ability to engage in daily activities are the rewards of prompt intervention.
Reducing Health Risks: Addressing CLI promptly not only safeguards the limb but also reduces the risk of secondary complications, such as infections and sepsis, which can be life-threatening.
In CLI, time is of the essence. Seeking medical help at the first sign of symptoms can lead to better outcomes and a brighter future for individuals affected by this condition.
Prevention Is Key
Preventing Critical Limb Ischemia (CLI) is undeniably preferable to managing its consequences. While not all risk factors can be eliminated, proactive steps can significantly reduce the likelihood of CLI development.
Managing Risk Factors: Smoking cessation, maintaining a healthy weight, controlling diabetes and high blood pressure, and keeping cholesterol levels in check are crucial in preventing CLI. Lifestyle changes can mitigate these risk factors.
Regular Check-ups: Regular medical check-ups, especially for individuals with risk factors, enable early detection and intervention. These routine visits allow healthcare providers to monitor vascular health and address any emerging issues promptly.
Education and Awareness: Knowledge is power. Understanding the symptoms and risk factors of CLI empowers individuals to recognize warning signs early and seek timely medical attention.
By prioritizing prevention, we can minimize the occurrence of CLI, reduce its impact on individuals and society, and ultimately save limbs and lives.
Regular medical check-ups can aid in early detection and management of CLI, especially for individuals with risk factors.
Critical Limb Ischemia may be a silent killer, but it doesn’t have to be. By understanding the warning signs, seeking timely professional help, and making necessary lifestyle changes, we can combat this condition effectively. Remember, prevention and early intervention are the keys to preserving limb health and quality of life.
FAQs
- What are the primary risk factors for Critical Limb Ischemia?
Answer: The primary risk factors for Critical Limb Ischemia (CLI) include smoking, diabetes, hypertension (high blood pressure), high cholesterol levels, and a history of cardiovascular disease. Age, obesity, and a sedentary lifestyle can also increase the risk. Understanding these risk factors is essential for early detection and prevention.
- Can CLI be reversed with treatment?
Answer: In many cases, CLI can be effectively managed with prompt and appropriate treatment, which can help improve blood flow to the affected limb and alleviate symptoms. However, the extent to which it can be reversed depends on the severity of the condition, how early it’s diagnosed, and the individual’s overall health. Timely intervention is crucial to prevent further deterioration and potential amputation.
- How can I recognize the difference between normal leg pain and CLI-related pain?
Answer: CLI-related pain is often more severe and can occur even during rest. It may be accompanied by other symptoms such as skin changes (pallor, coolness), slow-healing wounds, and ulcers. If you experience persistent, severe leg pain, especially if it worsens with activity and improves when you rest, it’s important to consult a healthcare professional for a proper evaluation.
- Are there any alternative therapies for CLI?
Answer: While the primary treatments for CLI typically involve lifestyle changes, medications, angioplasty, stenting, or bypass surgery, some individuals may explore complementary therapies like acupuncture, herbal supplements, or hyperbaric oxygen therapy. It’s crucial to discuss these options with a healthcare provider, as they should complement, not replace, evidence-based medical treatments.
- What is the long-term prognosis for individuals living with CLI?
Answer: The long-term prognosis for individuals with CLI varies based on factors such as the severity of the condition, the presence of underlying health issues, and the effectiveness of treatment. With timely intervention and appropriate management, many individuals can improve their quality of life, reduce the risk of amputation, and lead fulfilling lives. Regular follow-up care and adherence to medical advice are essential for a better prognosis.