Diabetes, a chronic condition affecting millions worldwide, is more than just high blood sugar. It’s a complex health issue that can lead to a range of severe complications. In this succinct yet informative article, we will delve into the various aspects of diabetes, from its types and causes to the common complications it can bring about. We’ll also discuss crucial management strategies and the importance of early detection. Whether you’re living with diabetes or seeking knowledge to support a loved one, this overview will provide you with valuable insights into this prevalent medical condition and how to navigate its challenges effectively.
Understanding Diabetes
Understanding diabetes is pivotal in managing this complex condition. Diabetes is primarily categorized into two types, each with distinct characteristics. Type 1 diabetes is an autoimmune disorder where the body’s immune system mistakenly attacks and destroys the insulin-producing cells in the pancreas. This typically occurs during childhood or adolescence, necessitating lifelong insulin therapy to regulate blood sugar levels.
Conversely, Type 2 diabetes, the more common form, is often linked to lifestyle factors. In Type 2 diabetes, the body either doesn’t produce enough insulin or becomes resistant to its effects. This type is closely associated with obesity, poor diet, sedentary habits, genetics, and a family history of diabetes.
Understanding these fundamental differences between Type 1 and Type 2 diabetes is essential, as it guides the approach to treatment and management. By recognizing the type of diabetes one has, individuals can work with healthcare professionals to develop tailored strategies for better blood sugar control and overall health.
Causes and Risk Factors
The causes and risk factors associated with diabetes are multifaceted and play a pivotal role in its development. While genetics can predispose some individuals to diabetes, lifestyle factors also significantly contribute to its onset.
Genetic Predisposition: Family history of diabetes can increase the likelihood of developing the condition. Specific genes may make some individuals more susceptible.
Obesity: Excess body weight, particularly around the abdomen, is a leading risk factor for Type 2 diabetes. Fat cells, especially in this area, can contribute to insulin resistance.
Poor Diet: Diets high in refined sugars, unhealthy fats, and low in fiber can contribute to diabetes. Consuming sugary beverages and processed foods can lead to weight gain and insulin resistance.
Lack of Physical Activity: A sedentary lifestyle can impair the body’s ability to regulate blood sugar levels, making it a significant risk factor.
Gestational Diabetes: Some women may develop diabetes during pregnancy, known as gestational diabetes. This condition increases the risk of Type 2 diabetes later in life.
Understanding these causes and risk factors empowers individuals to make informed choices about their lifestyle, thereby reducing the risk of diabetes and its associated complications.
Common Complications of Diabetes
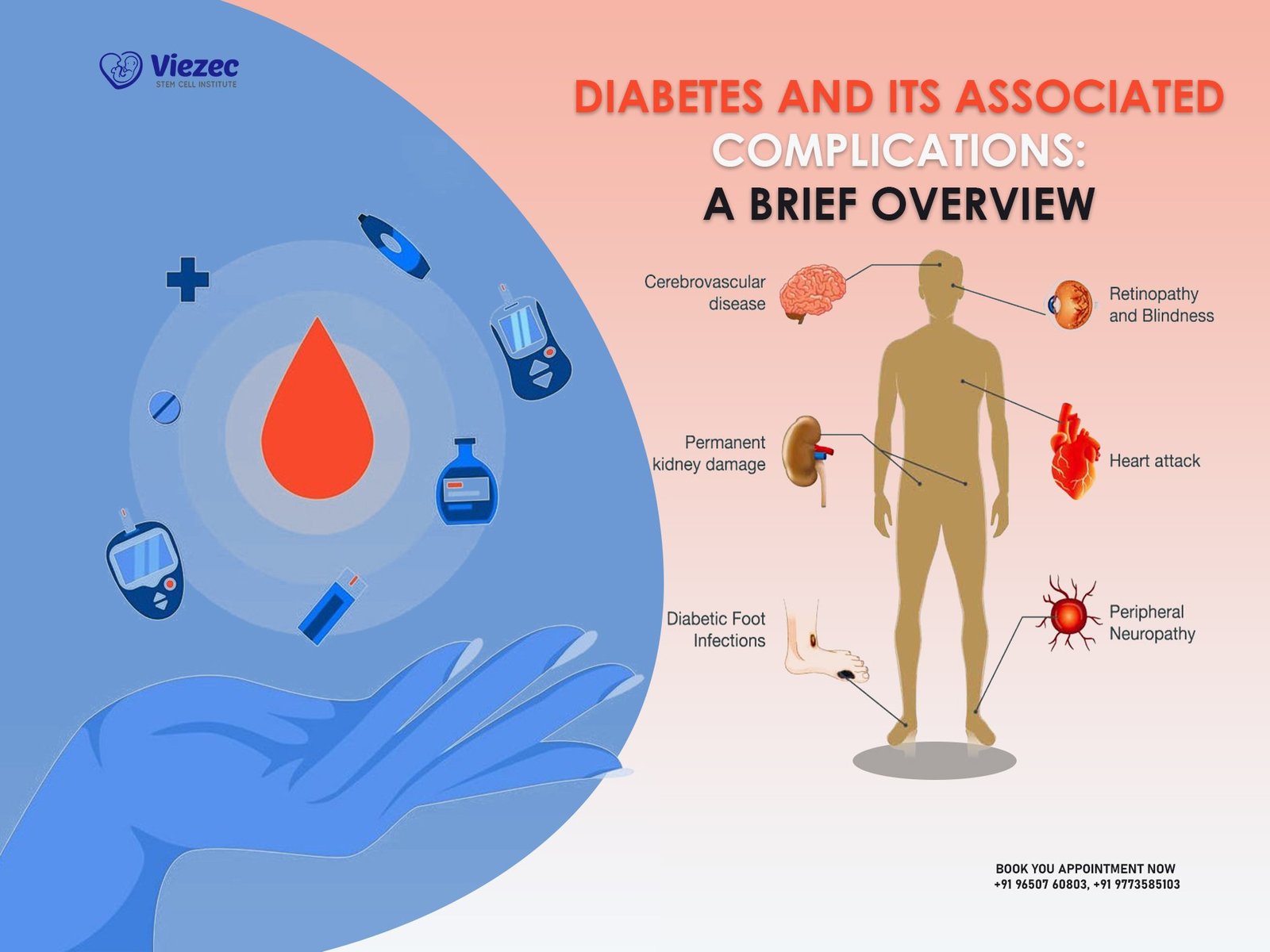
Diabetes, if not effectively managed, can lead to a range of debilitating and potentially life-threatening complications. Here are some of the common complications associated with this chronic condition:
Cardiovascular Complications: Diabetes significantly increases the risk of heart disease, including coronary artery disease, heart attacks, and strokes. High blood sugar levels can damage blood vessels and nerves, making the cardiovascular system vulnerable.
Neuropathy: Nerve damage due to diabetes, known as neuropathy, can lead to tingling, numbness, and pain, typically in the extremities. Severe cases may result in amputations.
Nephropathy: Over time, diabetes can damage the kidneys, leading to a condition called nephropathy. It can progress to chronic kidney disease or even kidney failure.
Retinopathy: Elevated blood sugar levels can harm the blood vessels in the retina, leading to a condition known as retinopathy. It can cause vision problems and, if left untreated, potentially lead to blindness.
These complications underscore the importance of vigilant diabetes management, including blood sugar control, regular medical check-ups, and a healthy lifestyle. Awareness and proactive measures can mitigate the risk of these severe complications, allowing individuals with diabetes to lead healthier lives.
Management and Prevention of Complications
Managing and preventing complications in diabetes is paramount for enhancing the quality of life and overall well-being of individuals living with this condition. Here are key strategies for managing and preventing diabetes-related complications:
Lifestyle Modifications: A healthy lifestyle is the cornerstone of diabetes management. This includes adopting a balanced diet rich in fruits, vegetables, whole grains, and lean proteins. Regular physical activity plays a vital role in regulating blood sugar levels, maintaining a healthy weight, and improving insulin sensitivity. Smoking cessation and limiting alcohol consumption are also essential components of a healthy lifestyle for diabetics.
Medications: In some cases, healthcare providers may prescribe medications to help manage blood sugar levels, blood pressure, and cholesterol. These medications can vary depending on the type of diabetes and individual health needs.
Regular Monitoring: Frequent monitoring of blood sugar levels is critical for tracking how well diabetes is being managed. Regular check-ups with healthcare providers enable early detection and intervention if complications arise.
Preventing complications involves not only managing blood sugar levels but also addressing other risk factors such as hypertension and dyslipidemia. By adhering to these management strategies, individuals with diabetes can reduce the risk of complications and enjoy a healthier, more fulfilling life.
Importance of Early Detection
The importance of early detection in diabetes cannot be overstated, as it can significantly influence the course of the disease and the prevention of complications. Here’s why early detection is crucial:
Regular Check-ups: Routine check-ups and screenings with healthcare professionals are essential for monitoring blood sugar levels and assessing overall health. Early detection allows for timely intervention and adjustments in treatment plans.
Prevention of Complications: Detecting diabetes in its early stages enables proactive measures to prevent or delay the onset of complications such as cardiovascular diseases, neuropathy, nephropathy, and retinopathy. Early management can help individuals maintain better control over their blood sugar levels, reducing the risk of complications.
Improved Quality of Life: Early detection and prompt intervention lead to better glycemic control, which can enhance the overall quality of life for individuals with diabetes. It helps in preventing symptoms from worsening and the need for more aggressive treatments.
Lifestyle Modifications: Early diagnosis provides an opportunity for individuals to make necessary lifestyle changes, such as adopting a healthier diet, increasing physical activity, and quitting smoking, which are vital components of diabetes management.
Early detection empowers individuals with diabetes to take control of their health, mitigate complications, and lead healthier, more fulfilling lives. Regular monitoring and proactive healthcare are key to achieving these positive outcomes.
Living Well with Diabetes
Living well with diabetes is entirely achievable with the right knowledge and proactive approach. Here are essential guidelines for individuals to thrive while managing this chronic condition:
Diet and Nutrition: Maintaining a balanced diet is paramount. Focus on portion control, complex carbohydrates, and high-fiber foods. Consultation with a registered dietitian can provide tailored meal plans and strategies for managing blood sugar levels effectively.
Exercise: Regular physical activity is a cornerstone of diabetes management. Engaging in activities like walking, swimming, or cycling can help control blood sugar levels, improve cardiovascular health, and boost overall well-being.
Stress Management: Stress can significantly affect blood sugar levels. Incorporate stress-reduction techniques such as meditation, yoga, or deep breathing exercises into your daily routine to help maintain stable glucose levels.
Regular Check-ups: Continual monitoring and regular check-ups with healthcare providers are essential to catch and manage complications early and adjust treatment plans as needed.
By embracing these principles and maintaining a proactive stance towards diabetes management, individuals can lead full, healthy lives and reduce the risk of complications associated with this condition.
Stem Cell Therapy and Diabetes
Stem cell therapy has emerged as a beacon of hope in the realm of diabetes management. This innovative approach harnesses the unique regenerative properties of stem cells to address the root causes of the disease. Stem cells, with their remarkable ability to transform into specialized cell types, hold the potential to replenish the pancreatic cells responsible for insulin production.
In the context of diabetes, stem cell therapy primarily revolves around two key objectives. First, it seeks to restore and enhance insulin production, helping individuals regain better control over their blood sugar levels. Second, it aims to mitigate the complications associated with diabetes, potentially preventing or slowing down the progression of issues affecting vital organs like the heart, kidneys, and eyes.
While research into stem cell therapy for diabetes is ongoing, early studies and clinical trials have shown promising results. This therapy may pave the way for more effective and holistic approaches to managing diabetes, offering renewed optimism to those living with this challenging condition. However, it’s essential to underscore that while stem cell therapy holds great promise, it is not yet a definitive cure, and further research and development are needed to unlock its full potential in the battle against diabetes.
Diabetes is a serious health condition that can have far-reaching consequences if not properly managed. Understanding the types, causes, and complications of diabetes is crucial for individuals with diabetes and their caregivers. By adopting a healthy lifestyle and seeking early medical intervention, individuals can reduce the risk of complications and lead fulfilling lives despite diabetes.
FAQs
- Can diabetes be cured?
- No, diabetes cannot be cured, but it can be effectively managed through lifestyle changes and medications.
- What is the best diet for someone with diabetes?
- A balanced diet with controlled carbohydrates and consultation with a dietitian is recommended.
- Are all diabetes complications preventable?
- While not all complications are preventable, early detection and proper management can significantly reduce the risk.
- How often should I check my blood sugar levels?
- The frequency of blood sugar monitoring depends on your doctor’s recommendations, but it’s typically several times a day for those on insulin.
- Can children develop type 2 diabetes?
- Yes, though it’s less common, children can develop type 2 diabetes, often due to obesity and genetic factors.