Diabetic Foot Ulcers (DFUs) are a pervasive and distressing complication faced by individuals living with diabetes. These open sores, primarily found on the feet, result from a combination of factors, including neuropathy, poor blood circulation, and a compromised immune system. Left untreated, DFUs can lead to severe infections and, in the worst cases, limb amputation. Conventional treatments, while valuable, often fall short in achieving comprehensive healing. However, there’s a ray of hope in the form of emerging stem cell-based solutions. Stem cell therapies have generated considerable excitement in the medical community for their potential to revolutionize the management of DFUs. This article explores the remarkable promise of stem cells in wound healing, the various types of stem cells used, clinical successes, challenges, and the role they may play in the future of DFU treatment. Join us on this journey through the exciting realm of regenerative medicine, where science and hope converge to improve the lives of those affected by diabetic foot ulcers.
Introduction to Diabetic Foot Ulcers
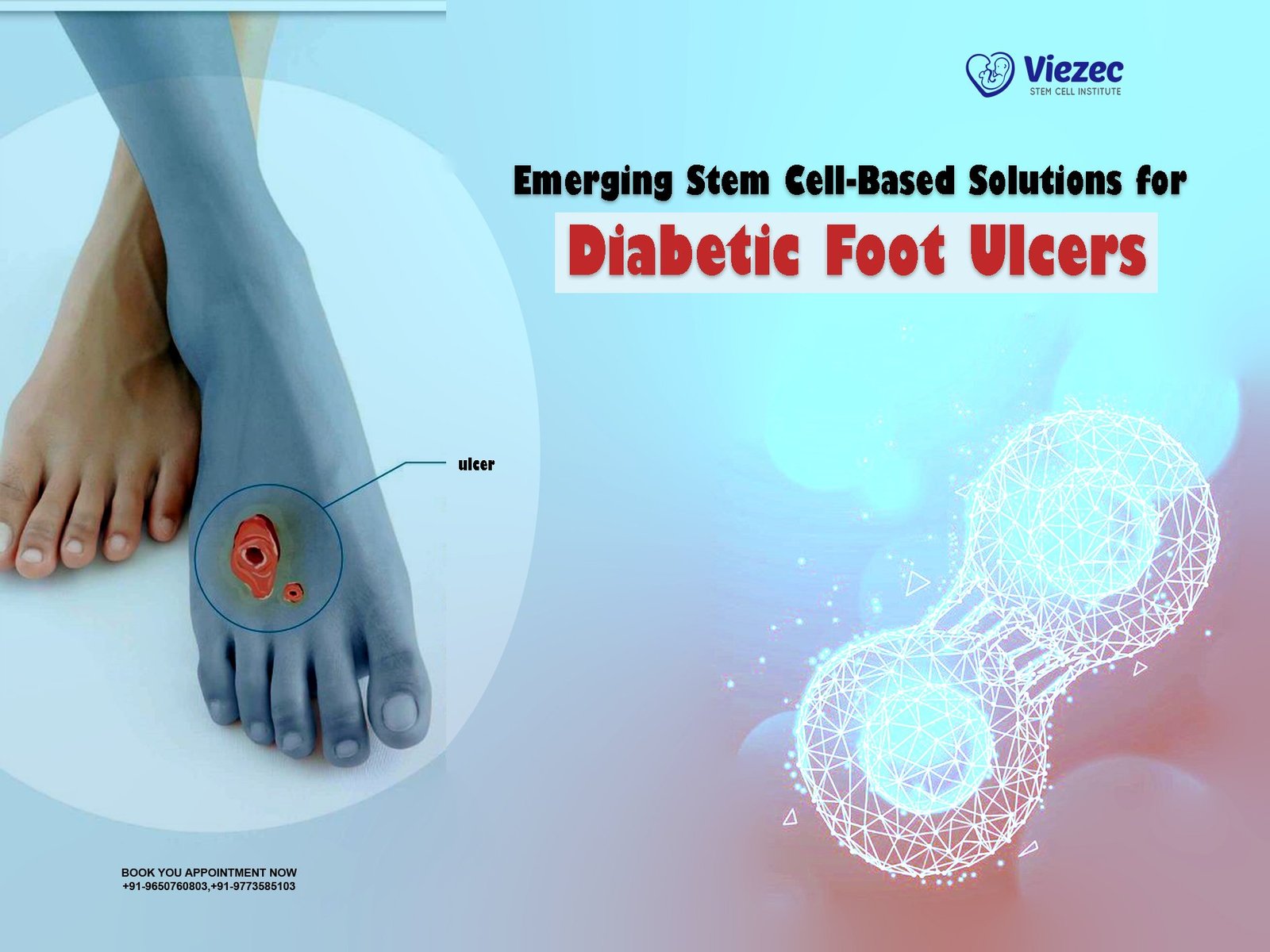
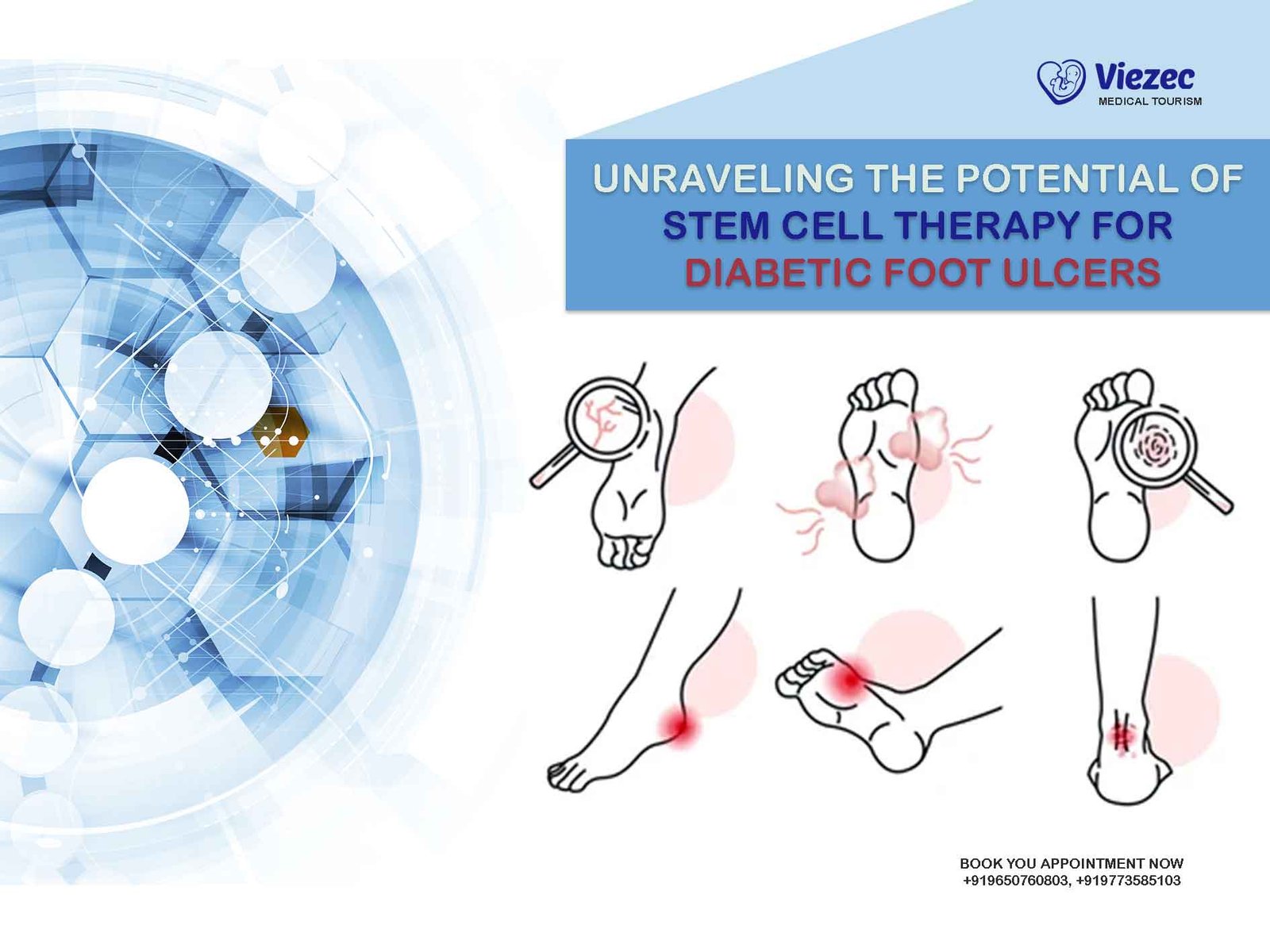
Diabetic Foot Ulcers (DFUs) are debilitating complications that afflict individuals with diabetes. These ulcers manifest as open wounds on the feet, resulting from a trifecta of neuropathy, poor blood circulation, and a weakened immune system. The convergence of these factors renders the feet susceptible to injuries, delayed healing, and potential complications. Beyond the physical pain and discomfort, DFUs pose a substantial global health concern. They can significantly reduce mobility, diminish the quality of life, and, if left unattended, may lead to the dire consequences of limb amputation. Understanding the nature and impact of DFUs is the first step towards exploring innovative solutions for their management.
Prevalence and Impact of Diabetic Foot Ulcers
The prevalence of Diabetic Foot Ulcers (DFUs) is a staggering global challenge, affecting millions of people living with diabetes. These ulcers exert a profound and far-reaching impact on individuals and healthcare systems alike. Beyond the immense personal suffering they cause, DFUs contribute to substantial economic burdens due to prolonged hospitalization, surgery, and ongoing medical care. The impact of DFUs goes beyond the physical; they lead to chronic pain, reduced mobility, and a compromised quality of life. Worse still, without proper management, DFUs can escalate to severe infections, gangrene, and amputations, making it imperative to explore innovative approaches for their effective prevention and treatment.
Conventional Treatments and Their Limitations
Conventional treatments have long been the mainstay in managing Diabetic Foot Ulcers (DFUs). They typically involve meticulous wound care, the use of antibiotics, and, in more severe cases, surgical interventions. While these approaches have offered some degree of success, they are not without their limitations. Often, conventional treatments struggle to achieve complete wound closure, especially in chronic cases. Moreover, they primarily address the symptoms rather than the underlying causes of DFUs, such as impaired circulation and neuropathy. The need for extended care and the risk of recurrence remain significant challenges, emphasizing the urgency of exploring advanced, more comprehensive solutions, including the exciting potential of stem cell-based therapies.
Promise of Stem Cell-Based Solutions
Amid the quest for innovative treatments, stem cell-based therapies have emerged as a beacon of hope in the management of Diabetic Foot Ulcers (DFUs). Stem cells possess extraordinary regenerative capabilities, making them a promising avenue for wound healing. These therapies involve harnessing the power of these versatile cells to promote tissue repair, reduce inflammation, and stimulate the regeneration of damaged skin. By targeting the root causes of DFUs, such as impaired circulation and neuropathy, stem cell-based solutions offer the potential for more effective and lasting results. This new frontier in regenerative medicine represents a paradigm shift, offering renewed optimism for individuals suffering from DFUs, paving the way for faster healing, reduced complications, and improved quality of life.
Types of Stem Cells Used in Treatment
Researchers exploring stem cell-based solutions for Diabetic Foot Ulcers (DFUs) have tapped into a diverse array of stem cell types to unlock their regenerative potential. Mesenchymal stem cells (MSCs), sourced from various tissues like bone marrow and adipose (fat) tissue, have taken center stage. Their versatility and ability to differentiate into various cell types make them invaluable in promoting tissue repair. Adipose-derived stem cells, in particular, are abundant and easily accessible. Additionally, induced pluripotent stem cells (iPSCs) have stirred intrigue due to their capacity to transform into any cell type. By understanding the unique attributes of these stem cell categories, researchers are refining their approach to tailor treatments that hold the promise of accelerated wound healing and enhanced recovery for DFU patients.
How Stem Cells Aid in Wound Healing
Stem cells play a pivotal role in the intricate dance of wound healing. Their regenerative prowess is harnessed in Diabetic Foot Ulcer (DFU) treatment to orchestrate a harmonious response. Stem cells secrete a myriad of growth factors, promoting cell proliferation and tissue regeneration. They also bolster vascularization by forming new blood vessels, facilitating improved blood flow to the affected area. Their immunomodulatory capabilities fine-tune the inflammatory response, reducing excessive inflammation and promoting a healing-conducive environment. This multifaceted approach addresses the core issues of DFUs, ultimately fostering accelerated recovery. The remarkable ability of stem cells to balance and optimize these processes underscores their potential to revolutionize wound healing for DFU patients.
Challenges and Safety Concerns
While stem cell therapies hold great promise, they are not without challenges and potential safety concerns. These include the risk of uncontrolled cell growth and the need for stringent quality control.
Regulatory Approvals and Future Prospects
Stem cell-based solutions for Diabetic Foot Ulcers (DFUs) are advancing through clinical trials and regulatory processes. As they gain approvals, the future of DFU treatment appears promising. With more therapeutic options on the horizon, there’s newfound hope for improved outcomes and a brighter outlook for individuals living with diabetes and struggling with the challenges of DFUs.
Role of Personalized Medicine
In the realm of Diabetic Foot Ulcer (DFU) treatment, personalized medicine emerges as a game-changer. This approach tailors therapeutic interventions to the unique characteristics and needs of each patient. Personalized medicine recognizes that no two DFU cases are identical and aims to optimize treatment outcomes. By considering individual variables such as the patient’s specific health conditions, genetics, and responsiveness to treatment, a more precise and effective strategy can be crafted. This personalized approach minimizes adverse effects, maximizes the chances of successful wound closure, and enhances the overall quality of care, marking a significant advancement in the management of DFUs.
Combining Stem Cell Therapy with Other Approaches
In the pursuit of comprehensive Diabetic Foot Ulcer (DFU) management, a multi-faceted approach emerges as a promising strategy. Combining stem cell therapy with other techniques, such as advanced wound care, creates a synergistic effect. This approach optimizes wound healing by addressing both the underlying causes and the symptoms of DFUs. By integrating regenerative power with established methodologies, patients can benefit from a well-rounded treatment plan that offers the best chance of achieving complete healing and preventing DFU recurrence.
Importance of Early Intervention
Early diagnosis and intervention are crucial in managing DFUs effectively. Timely treatment can prevent complications and improve overall patient outcomes.
Stem cell-based solutions offer new hope in the battle against Diabetic Foot Ulcers. While challenges remain, ongoing research and clinical trials are paving the way for more effective and personalized treatment options. With advancements in regenerative medicine, the future looks promising for individuals living with diabetes and DFUs.
Frequently Asked Questions
Are stem cell-based treatments the only option for managing diabetic foot ulcers?
No, while stem cell therapies show promise, there are other conventional treatments and advanced wound care techniques available. The choice of treatment depends on the individual patient’s condition and preferences.
Are stem cell therapies covered by health insurance?
Insurance coverage for stem cell therapies can vary. It’s essential to check with your insurance provider to determine whether these treatments are covered under your policy.
What are the potential risks associated with stem cell-based DFU treatment?
Some risks include uncontrolled cell growth, infection, and the need for quality control to ensure the safety of the treatment. Discuss these concerns with your healthcare provider.
How long does it typically take to see results from stem cell-based treatments for DFUs?
The timeline for results can vary from patient to patient. Some may experience improvements within weeks, while others may take several months. Patience is essential in the healing process.
Can stem cell therapy be combined with other treatments for diabetic foot ulcers?
Yes, it’s possible to combine stem cell therapy with other approaches like advanced wound care. This combination can enhance the overall effectiveness of treatment.